Supportive care
Paediatric Chordoma Guide
Supportive care is an important part of care for people with serious illnesses like cancer. Supportive care aims to improve quality of life for your child and family before, during and after treatment. This broad term covers management of physical symptoms, such as pain and nausea, and other aspects such as nutrition and mental wellbeing.
The MDT will work extremely hard to keep your child as comfortable and as symptom free as they can during treatment. In many parts of the UK, children with cancer are referred to the local children’s hospice team. This team can provide specialist and expert care and advice in the management of your child’s symptoms. This can be very beneficial as it can help make your child more comfortable whilst on treatment. Supportive care from a hospice team doesn’t mean that your child won’t get better.
Supporting your child through cancer is understandably one of the most difficult things a parent can go through and can affect your physical, emotional and financial wellbeing. Don’t think you have to go through this alone – there is support available and accepting support when needed can help make this very difficult time easier for you and your child.
Words in bold are explained in a glossary.
Paediatric Chordoma Guide
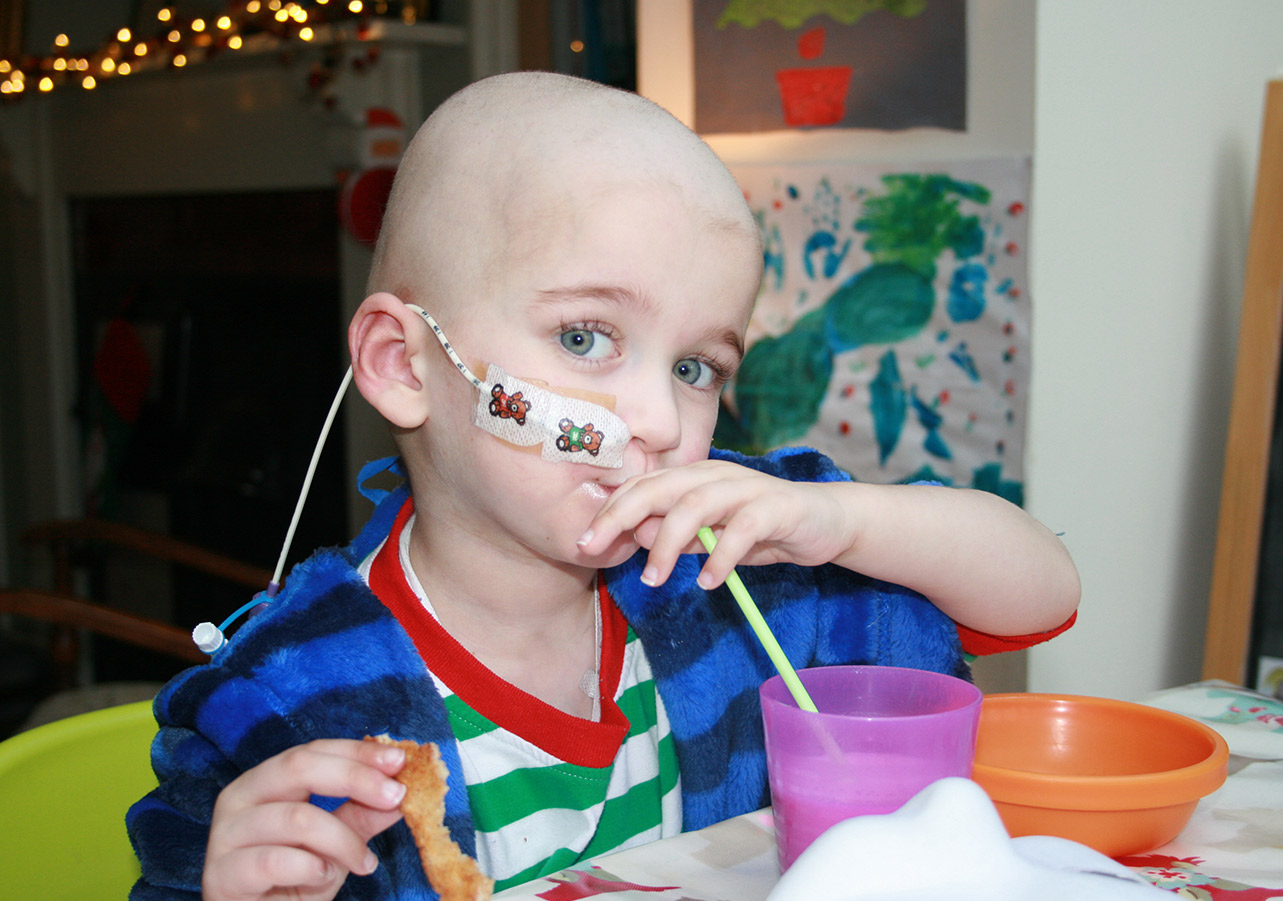
If your child needs help with feeding
Unfortunately, it is possible that the treatments that your child has for their chordoma will make them feel sick, alter their sense of taste or make swallowing difficult. This can mean that they can struggle to eat enough food to give their bodies the necessary nutrients and calories. This may especially be the case if they are very young.
You and the doctors can try and encourage calorie intake with small, frequent meals and high energy snacks. However, if your child is becoming increasingly upset at the thought of eating, or is not managing to maintain their weight, the team caring for them are likely to recommend a feeding tube is fitted.
The benefits of feeding tubes are that children can receive food directly into their stomach when they feel unable to eat. Feeding tubes can also make it easier for your child to take any unpleasant-tasting oral medications, as they can also be passed through the tube.
Nasogastric (NG) tubes are thin, soft tubes that are passed through your child’s nostril, down their throat and into the stomach. Once inserted, they remain in place, held by tape on your child’s cheek.
Inserting the NG tube is usually quick and easy. It doesn’t hurt, but your child might feel a brief amount of discomfort as the tube is inserted. Once in place it is something most children get used to very quickly.
NG tubes are designed for short-term use. The tube will need to be replaced and swapped to the other nostril after about a month.
PEG stands for percutaneous endoscopic gastrostomy, a procedure in which a flexible feeding tube is inserted directly into your child’s stomach via a small incision. The procedure is usually carried out under a general anaesthetic.
PEG tubes are designed for long-term use. They are often used if your child has been reliant on an NG tube for a while and is likely to need a feeding tube in the longer-term. They last for several months before they need to be replaced.
In rarer circumstances, Total Parenteral Nutrition (TPN) may be suggested.
TPN is a form of liquid food given directly into the bloodstream. TPN allows nutrition to be given in circumstances when your child’s intestines (gut) might not be working very well (for example due to side effects of chemotherapy). TPN delivers a solution of nutrients directly into a vein, either continuously or overnight, preferably through a central line. The line is placed under the skin and into a vein leading to the heart. The other end comes out through a small incision in your child’s chest. It is inserted and removed under general anaesthetic.
TPN is usually only used when other methods, such as NG or PEG feeding, have been tried and failed to deliver enough nutrition for your child.
Your child’s team will talk through all of the feeding options with you should your child need help with feeding.
Dealing with loneliness and isolation
Cancer and its treatments can weaken your child’s immune system so that they may need to spend some time away from public places, including school and their friends. Isolation can be particularly hard for children. There might be times during your journey that you also feel alone. The challenges of cancer can understandably place a substantial mental burden on children and their families. It is important to remember that you are not alone and there are people who you can talk to for advice and support.
Resources: